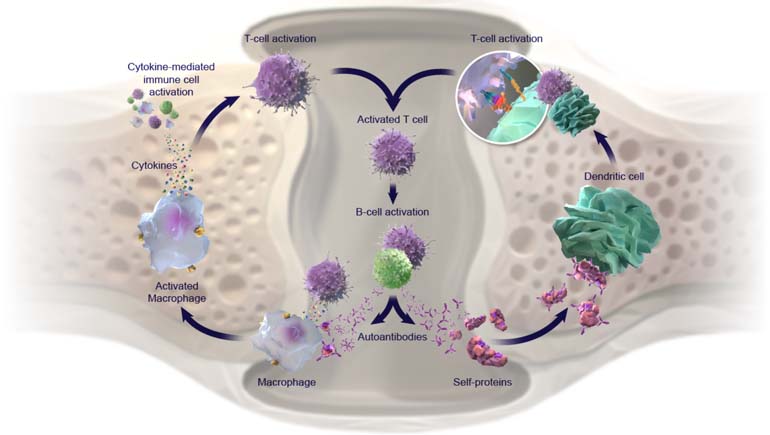
A biomarker is a measurable indicator of a normal or pathologic biological process, or an indicator of response to therapy. As such, biomarkers have generated significant interest within the immune-mediated disease research and medical communities because of their potential to help physicians make predictions about disease progression, and to serve as guides for therapeutic decision making. In the future, biomarkers, may be used to inform personalized treatment strategies, i.e., "road maps" – disease management plans for individual patients that can be followed and revised over time. Bristol Myers Squibb's research focus is on unlocking the full potential of these precision medicine approaches to patient care, in order to get to a destination where we can improve and/or optimize outcomes for people living with immune-mediated diseases.
Bristol Myers Squibb’s journey in this area began 20 years ago when we pioneered the science of modulating the body's immune response to treat diseases with our rheumatoid arthritis research. Rheumatoid arthritis is an immune-mediated disease that causes joint damage with chronic pain, stiffness and swelling of joints. Our research was grounded in the understanding that rheumatoid arthritis could present and behave very differently in different individuals. We therefore worked to identify a different approach to treatment.
Along the way, we've uncovered insights about people who have a more highly active and progressive form of the disease, which can lead to worse outcomes. These patients frequently test positive for a biomarker called anti-citrullinated protein antibody, or ACPA. ACPA, which is found in 70-90 percent of rheumatoid arthritis patients, can be detected in a person's bloodstream before joint damage becomes clinically apparent, offering physicians important. predictive information.
At Bristol Myers Squibb, we’re proud to be a part of advancing the scientific understanding of the pathophysiology of rheumatoid arthritis and of the value of key biomarkers in the prognosis and treatment of this disease, and our work isn't stopping there. Our aspiration is to deliver life-changing medicines tailored for individual patients across a range of immune-mediated diseases. Patient-targeted therapies could help deliver higher rates of remission and better outcomes in diseases like lupus and ulcerative colitis, among others, where unmet needs persist and patients continue to seek improvements, despite available therapies.
Our scientists are inspired by this vision every day as they conduct immunology research and are leveraging foundational research in RA as they strive to develop new patient-targeted therapies. Examples of our research include:
- Systemic lupus erythematosus, referred to as SLE or lupus, causes systemic inflammation affecting multiple organs, including skin, joints, kidneys, heart and brain. Our research is exploring targets based on a number of approaches, including the pathophysiology of the disease, patient pathotypes, among others.
- Psoriasis and psoriatic arthritis are chronic, immune-mediated conditions. Psoriasis is characterized by a rapid, unpredictable production of skin cells, which leads to the formation of painful scaling and plaques. Psoriatic arthritis impacts the joints and skin. Bristol Myers Squibb is pursuing a novel therapy with a unique, selective mechanism of action because many patients still struggle with insufficient disease control and continue to be undertreated.
- Inflammatory bowel disease, which includes ulcerative colitis and Crohn’s disease, causes swelling or inflammation of the intestines, which may result in permanent damage and can severely impact the everyday life of patients. Our research is exploring targets based on the pathophysiology of the disease to advance care and improve treatment outcomes for patients.
Our scientists are passionate in their pursuit of novel therapies that have the potential to improve outcomes and expand therapeutic options for patients with immune-mediated diseases.
Our hope is that as our research continues, we’ll be able to open up even more opportunities for the discovery of novel biomarkers in immune-mediated diseases, and get closer to our goal of advancing personalized approaches to treatment strategies so that the "right treatment is provided to the right patient at the right time." Treatment discovery and improvement can be a long road with many twists and turns. Our scientists are committed to leveraging our expertise in drug discovery and translational medicine, as well as the latest biomarker science, to help get to a place where we can improve the lives of those touched by immune-mediated diseases.
Subscribe to Our stories alerts
Beyond just relevant information about Bristol Myers Squibb's therapeutic areas and innovation, Our stories offer a window into the work our employees do every day for patients.
About Bristol Myers Squibb
Bristol Myers Squibb is a global biopharmaceutical company whose mission is to discover, develop and deliver innovative medicines that help patients prevail over serious diseases. As global citizens, we work sustainably and responsibly to create a positive impact in the communities where we live and work.