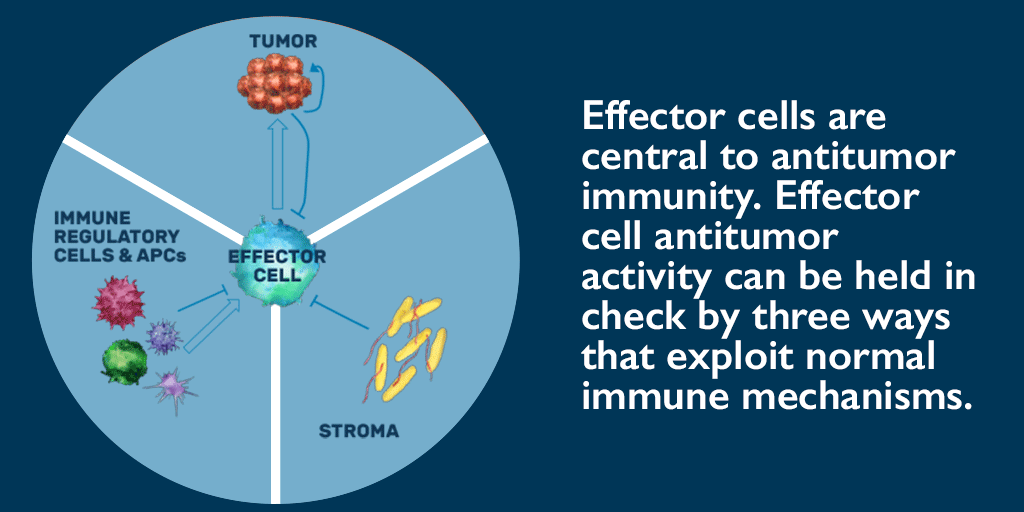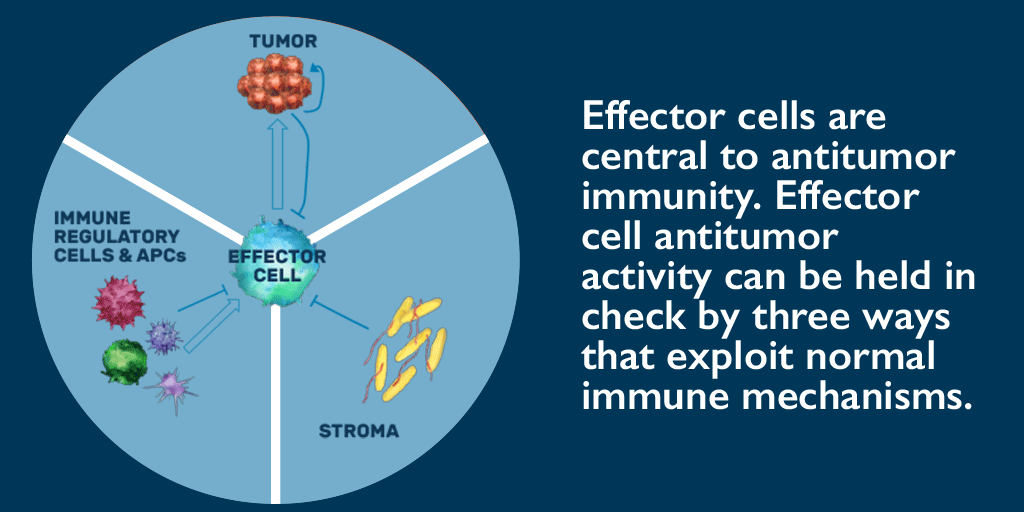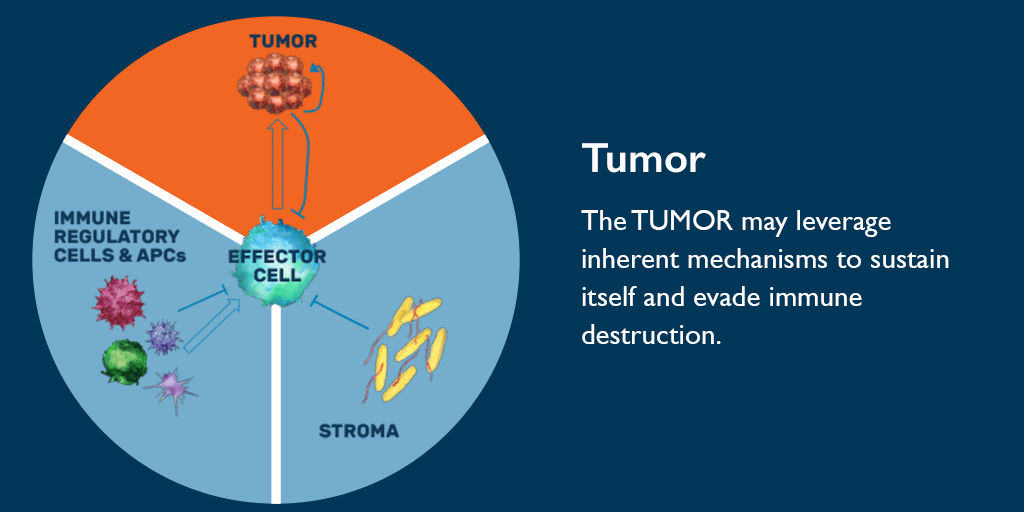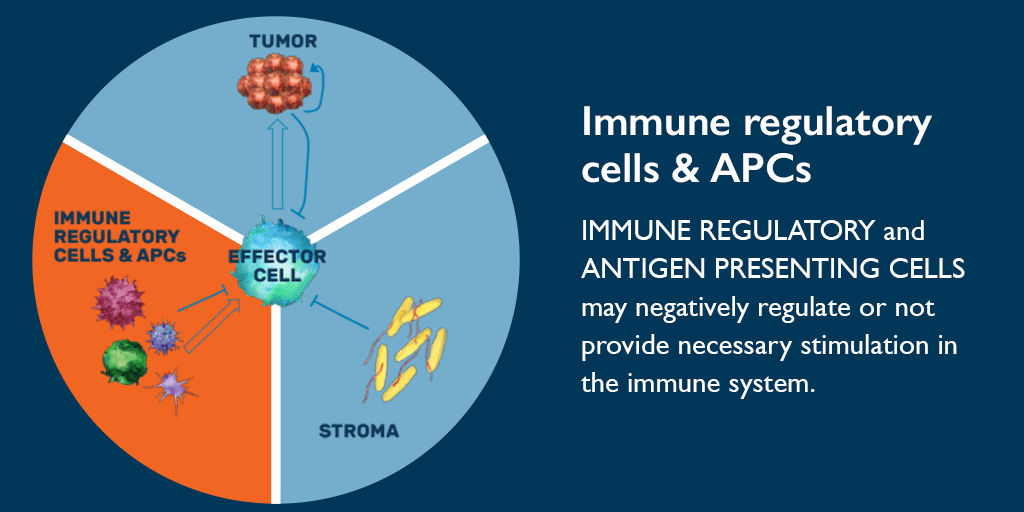
IL-2 is a cytokine for activating T cells and natural killer (NK) cells. Selectively stimulating the βγ IL-2 receptor found only on the surface of T cells and NK cells can increase expansion and cytotoxic activity of both T cells and NK cells. This creates inflammation in the tumor microenvironment and recruits additional immune cells to the site. The increased number of T cells in a tumor (also known as tumor-infiltrating lymphocytes, or TILs) is important for stimulating an anti-tumor immune response. Once in the microenvironment, T cells can bind to the tumor cells and attack them at the source.
“IL-2 is an established mechanism that acts to increase the quantity and the quality of T cells,” says Vicki Goodman, head of New Asset Development at Bristol Myers Squibb. “By essentially stepping on the gas pedal of the immune system, selective stimulation of IL-2 receptors could have an impact across a broad range of tumors, including those which are not generally sensitive to checkpoint inhibition.”
Identifying Rational Combinations to Fight Cancer
Most tumors use multiple mechanisms of immune suppression, which may evolve as the disease progresses. Knowing this, Bristol Myers Squibb is investigating how signaling pathways interact to identify optimal treatment combinations (doublet and/or triplet) to activate the strongest anti-tumor response.
Researching IL-2 and PD-1 in combination, for instance, may be a key strategy to more effectively activate the anti-tumor immune response, including in some patients who are not otherwise responsive to PD-1 inhibitors. Activation of the innate immune system or activating co-stimulatory pathways may also be complementary approaches with IL-2 activation for some tumors.